What are mouth ulcers?
Mouth ulcers commonly appear as round or oval sores that develop just after you’ve damaged or irritated the soft moist skin lining the inside of your mouth (called the mucosal membrane). They can be white, red, yellow or grey in colour and look like small craters with swollen, raised edges.
There are lots of nerves close to the skin’s surface in your mouth, which means that mouth ulcers can be very painful. Everyday things such as eating and drinking can irritate the sores and it can be painful just to chew food or brush your teeth.
When untreated, mouth ulcers will usually heal themselves within 7 to 10 days.

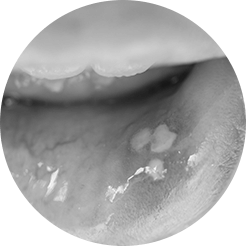

What causes mouth ulcers?
Mouth ulcers are a common problem, but we don’t always know the reasons why they develop.
Most mouth ulcers are often the result of accidental damage to the lining of your mouth through things such as:
- Biting your lip, tongue or cheek
- Slipping with your toothbrush and bumping the inside of your mouth or gums
- Damage form a sharp tooth or filling
- Rubbing of ill-fitting dentures or braces
- Eating hard or sharp-edged foods
- Burning your mouth with hot food or drinks
Other causes can include:
- Infections such as cold sores, chicken pox, shingles and oral thrush
- Food allergies
- Certain medications or medical treatments – such as non-steroidal anti-inflammatory drugs (NSAIDs), beta blockers, chemotherapy or radiotherapy.
Some people are more prone to getting reoccurring ulcers (called aphthous ulcers). The reason why these ulcers keep returning is not always clear but it is thought that certain things can act as triggers, such as:
- Stress or anxiety
- Hormonal changes – particular during a woman’s monthly period or during pregnancy
- A poor diet – which may lead to nutritional deficiencies such as vitamin B12, iron or folic acid
- Beginning to quit smoking cigarettes
- Having a gastrointestinal disease such as Crohn’s or coeliac disease
- Your genes – having ulcers can sometimes run in families!
How to treat mouth ulcers
Most mouth ulcers will usually heal up and go way in a couple of weeks. In the meantime, here are a few things you can try to help manage any painful symptoms:

Avoid eating anything that will irritate your ulcer and make the pain worse, such as hard, spicy or sour foods

Drink lots of cool fluids – try using a straw to keep the liquids away from the painful areas

Give you mouth a regular rinse out with warm, slightly salty water

Try to keep your mouth clean – use a soft toothbrush and brush gently
If your ulcer becomes very painful then you may want to use some form of medication. The main aim of any treatment is to lessen the pain or discomfort caused by the ulcer and help promote healing. The type of medication you use will depend on how much pain and discomfort you are in and what may have caused your ulcer and can include:
- Pain-relieving mouthwashes, sprays or gels (available from your pharmacy) to help reduce the pain in the area directly around your ulcer. These usually only work for a short time.
- Medicated antiseptic mouthwashes such as those containing chlorhexidine gluconate (available from your pharmacy) reduce the build up of bacteria in your mouth and help prevent your ulcer becoming infected.
- Steroid-containing* protective pastes, such as Kenalog in Orabase®, provide rapid pain relief by reducing the inflammation associated with ulcers. The paste also forms a protective film over the ulcer, protecting it from further irritation and damage, providing an environment for accelerated healing. Kenalog in Orabase® is available from your local pharmacy without a prescription after consultation with your pharmacist.
*Steroid-containing medications are not suitable if you have a viral, bacterial or fungal infection in your mouth or throat as they can make these infections worse.
Preventing mouth ulcers
Preventing mouth ulcers can be a bit tricky when the cause is not known or is out of your control, but there are a few things you can do to reduce the likelihood of them developing:
- Remember to take care and brush your teeth gently with a soft toothbrush
- Eat a healthy well-balanced diet
- Keep any underlying medical conditions well-controlled
- See your dentist about any broken teeth, rough surfaces, or ill-fitting dentures
- Make sure your dentures or braces are not broken and fit properly

Cold sore vs ulcer
Not sure whether cold sores and mouth ulcers are the same thing? Both are common, painful mouth problems, but the two are quite different and it’s important not to confuse them as they need to be treated differently.
What is a cold sore?
Cold sores are extremely contagious blisters that appear when you have a herpes simplex virus (or HSV) infection.
When a cold sore blister is on its way, you may start to feel a tell-tale tingling or burning around your mouth.
A cluster of small, fluid filled blisters then usually appear, either on the outside of your lips or around your mouth – although they can also sometimes be found elsewhere on your body.
The blisters can grow bigger and become painful, they can also bust and leak contagious fluid before crusting over.
Cold sores are very contagious and are easily spread from person to person. They remain contagious until they have healed completely – so it’s important to remember to avoid any close contact with other people until your cold sore has disappeared.
Once you have a HSV infection cold sores can be triggered periodically by things such as being tired or sun exposure.
Are ulcers in the mouth contagious?
You may not be able to pinpoint exactly what caused your mouth ulcer to suddenly appear – but it’s comforting to know that mouth ulcers are not contagious. However, mouth ulcers can sometimes be confused with cold sores which are very contagious.
Although some people are more prone to getting mouth ulcers and may get them regularly, it doesn’t mean they have ‘caught’ their ulcer from someone, and they cannot pass it on to someone else either.
How long do mouth ulcers take to heal?
Mouth ulcers can be annoyingly common, irritating and painful – and may feel like they’re taking ages to clear up – but the good news is, most ulcers will clear up by themselves in 1-2 weeks.
To give you an idea of what’s going on as an ulcer heals, here’s a timeline for one caused by biting your cheek:
- Day 1: Within seconds of biting yourself, your immune system kicks-in, blood vessels narrow, and clots form to stop any bleeding
- Days 1-3: Over the next few days, the spot becomes inflamed – turns red, swells up and starts to hurt – and the typical whitish ulcer forms
- Days 4-6: The ulcer reaches its final size, then starts to heal and get smaller, and the pain begins to fade away
- Days 7-14: The ulcer has healed and usually disappears completely without leaving a scar.
The actual time it takes for an ulcer to heal will vary depending on things such as the ulcer’s size or what caused it. Most ulcers are only small (less than 5mm in diameter) and will usually heal faster than larger ulcers.
If your mouth ulcer takes longer than 3 weeks to heal, is becoming more painful or you keep getting ulcers – then it’s a good idea to talk to your doctor or dentist and get things checked out.
When your ulcer makes eating and drinking a problem:
- try eating soft foods that need less chewing;
- stay away from hard or sharp food, such as crisps or crusty bread, that may cause more pain and damage;
- use a straw to keep liquids away from your ulcer;
- avoid hot, salty, acidic or spicy food and drinks that may make your ulcer worse.
When brushing your teeth:
- use a soft-bristled toothbrush to help prevent any more discomfort or damage;
- don’t use a toothpaste that contains sodium lauryl sulphate.
When you need help finding relief:
- ask your pharmacist about using Kenalog in Orabase® . This triple action dental paste heals mouth ulcers rapidly, forms a protective barrier over the ulcer to help protect against rubbing and irritation and is effective in suppressing the recurrence of mouth ulcers;
- try using an antiseptic mouthwash to help prevent infection of the ulcer that may slow the healing process;
- do other simple things like rinsing your mouth with salt water, which can also help relieve pain and reduce the chance of your ulcer becoming infected.